Journal Description
Société Internationale d’Urologie Journal
Société Internationale d’Urologie Journal
(SIUJ) is an international, peer-reviewed, open access journal that covers all aspects of urology and related fields. The journal is owned by the Société Internationale d’Urologie (SIU) and is published bimonthly online by MDPI (since Volume 5, Issue 1 - 2024).
- Open Access— free for readers and authors (diamond open access), with article processing charges (APC) paid by the Société Internationale d’Urologie.
- Rapid Publication: first decisions in 16 days; acceptance to publication in 5.8 days (median values for MDPI journals in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
subject
Imprint Information
Open Access
ISSN: 2563-6499
Latest Articles
Protocol for the RoboSling Trial: A Randomised Study Assessing Urinary Continence Following Robotic Radical Prostatectomy with or without an Intraoperative Retropubic Vascularised Fascial Sling (RoboSling)
Soc. Int. Urol. J. 2024, 5(2), 148-159; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020024 - 17 Apr 2024
Abstract
►
Show Figures
Objectives: To determine if early (three months) and late (one year) post-operative continence is improved by performing a novel retropubic vascularised fascial sling (RoboSling) procedure concurrently with robot-assisted radical prostatectomy in men undergoing treatment for localised prostate cancer. To additionally assess surgical outcomes,
[...] Read more.
Objectives: To determine if early (three months) and late (one year) post-operative continence is improved by performing a novel retropubic vascularised fascial sling (RoboSling) procedure concurrently with robot-assisted radical prostatectomy in men undergoing treatment for localised prostate cancer. To additionally assess surgical outcomes, quality of life and health economic outcomes in patients undergoing the novel RoboSling technique. Methods: This study aims to recruit 120 consecutive patients with clinically localised prostate cancer who have chosen to undergo robot-assisted radical prostatectomy in the Sydney Local Health District, Australia. A prospective assessment of early and late post-operative continence following robot-assisted radical prostatectomy with and without a RoboSling procedure will be performed in a two-group, 1:1, parallel, randomized controlled trial. Four surgeons will take part in the study, all of whom are beyond their learning curve. Patients will be blinded as to whether the RoboSling procedure is performed for them, as will be the research officers collecting the post-operative data on urinary function. Trial Registration: ACTRN12618002058257. Results: The trial is currently underway. Conclusions: The RoboSling technique is unique in that the sling is vascularised and has a broad surface area compared to previously described slings in the literature. If a clinically significant improvement in post-operative continence is established with the RoboSling, then, we can in turn expect improvements in quality of life for men undergoing this technique with radical prostatectomy.
Full article
Open AccessUrology around the World
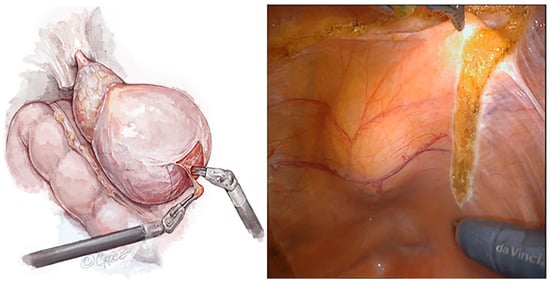
Robot-Assisted Surgery in Poland: The Past, the Present, and the Perspectives for the Future
by
Roman Sosnowski, Krzysztof Jakubiak, Hubert Kamecki, Grzegorz Kade, Tomasz Drewa, Tomasz Szydełko, Piotr Chłosta, Piotr Kania and Piotr Jarzemski
Soc. Int. Urol. J. 2024, 5(2), 142-147; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020023 - 16 Apr 2024
Abstract
►▼
Show Figures
In recent decades, we have been witnessing a technological revolution in the area of minimally invasive urologic surgery, with robot-assisted surgery being one of the most game-changing inventions [...]
Full article
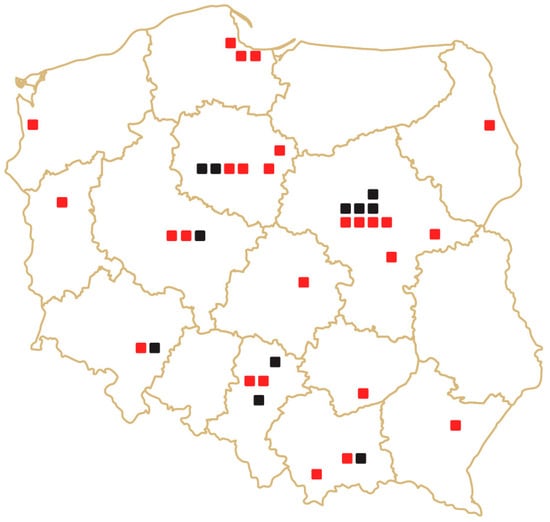
Figure 1
Open AccessSystematic Review
Systematic Review: Seventy-Seven Cases of Signet Ring Cell Adenocarcinoma of the Bladder
by
Kenneth Keen Yip Chew, Madison Boot, Katelyn Wilson, Cameron Sowter, Wei Xuan, Raymond Stanton and Paul Bergamin
Soc. Int. Urol. J. 2024, 5(2), 133-141; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020022 - 16 Apr 2024
Abstract
►▼
Show Figures
Background: Signet ring cell adenocarcinoma (SRCC) of the bladder is a rare and aggressive histological subtype of bladder cancer. Due to its infrequency, the understanding of its clinical behaviour, treatment strategies, and outcomes remains limited, being primarily derived from isolated case reports
[...] Read more.
Background: Signet ring cell adenocarcinoma (SRCC) of the bladder is a rare and aggressive histological subtype of bladder cancer. Due to its infrequency, the understanding of its clinical behaviour, treatment strategies, and outcomes remains limited, being primarily derived from isolated case reports and series. Objective: To systematically review and analyse the available literature on SRCC of the bladder, emphasizing its clinical characteristics, diagnostic approaches, treatment modalities, and outcomes. Material and Methods: A comprehensive search was conducted across PubMed, Embase, and Medline following the PRISMA guidelines, including case reports, case series, observational studies, and clinical trials reporting on bladder SRCC. Results: We included 38 articles reporting on 77 patients, primarily males (79.2%), with a median age of 64 years. The most common presenting symptoms were haematuria (64.8%) and lower urinary tract symptoms (46.3%). All the diagnoses were based on histopathological examination of bladder tissue samples and immunohistochemistry. Mixed histological types of bladder cancer were found in 20.7% of cases, most commonly urothelial carcinoma (61.1%). The treatments varied, with 53.2% of patients undergoing radical cystectomy, 24.7% receiving radiotherapy, and 16.9% receiving chemotherapy. The five-year survival rates were 9.4%. Conclusion: Bladder SRCC presents aggressively, with varied treatment strategies; however, radical cystectomy appears to be the optimal means of surgical management for organ-confined disease. The overall survival rate is low, highlighting the need for further research to understand and manage this rare bladder cancer variant. All patients should undergo evaluation to exclude extravesical primaries. This systematic review contributes to a better understanding of this disease and may guide clinical management strategies.
Full article

Figure 1
Open AccessArticle
Role of Multiparametric Magnetic Resonance Imaging and Targeted Biopsy in the Detection of Clinically Significant Prostate Cancer in Patients with Suspicious Digital Rectal Examination
by
Vincenzo Ficarra, Alessandro Buttitta, Marta Rossanese, Angela Alibrandi, Giuseppina Anastasi, Alfredo Blandino, Antonio Ieni, Maurizio Martini and Gianluca Giannarini
Soc. Int. Urol. J. 2024, 5(2), 122-132; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020021 - 16 Apr 2024
Abstract
►▼
Show Figures
Objectives: Few studies have examined the role of prostate MRI in patients with suspicious digital rectal examination (DRE) and/or PSA > 10 ng/mL. In a cohort of non-screened patients with suspicious DRE, we investigated the rate of avoidable prostate biopsies and potentially
[...] Read more.
Objectives: Few studies have examined the role of prostate MRI in patients with suspicious digital rectal examination (DRE) and/or PSA > 10 ng/mL. In a cohort of non-screened patients with suspicious DRE, we investigated the rate of avoidable prostate biopsies and potentially missed clinically significant prostate cancer (csPCa) with negative MRI, and the concordance between targeted biopsy (TBx) and systematic biopsy (SBx) in detecting csPCa with positive MRI. Methods: We retrospectively examined 199 biopsy-naïve patients with suspicious DRE who underwent prostate MRI before transperineal biopsy. Prostate Imaging—Reporting and Data System (PI-RADS) v2.1 ≥ 3 category of the index lesion defined a positive MRI. Combined TBx/SBx and SBx alone were performed for positive and negative MRI, respectively. An International Society of Urogenital Pathology Grade Group ≥ 2 defined csPCa. We calculated the csPCa detection rate of TBx, SBx, and combined TBx/SBx. The Cohen kappa statistic was used to measure the concordance between TBx and SBx. Results: Ninety-one (45.7%) csPCa cases were detected. MRI was positive in 153 (76.9%) patients. In the 46 patients with negative MRI, SBx detected 5 (10.9%) csPCa cases. Prostate biopsy could, thus, be avoided in 41/199 (20.6%) patients at the cost of missing 5/91 (5.5%) csPCa cases. The concordance between TBx and SBx in detecting csPCa with positive mpMRI was substantial (k = 0.70). Specifically, 6/86 (6.9%) csPCa cases were detected with TBx, and 17/86 (19.7%) with SBx alone. Concordance was almost perfect (k = 0.82) in patients with PSA > 10 ng/mL. Only 4/38 (10.5%) csPCa cases were missed by TBx, and only 1 (2.6%) csPCa case was identified by TBx alone. Conclusions: MRI in patients with suspicious DRE could avoid roughly 21% of unnecessary biopsies at the cost of missing approximately 6% of csPCa cases. Moreover, MRI and TBx complemented SBx in detecting csPCa in the subgroup with PSA > 10 ng/mL.
Full article

Figure 1
Open AccessArticle
Rectal Spacer Reduces Gastrointestinal Side Effects of Radiation Post Radical Prostatectomy
by
Anne Hong, Damien Bolton, Trung Pham, David Angus, David Pan, Daryl Lim Joon, Alwin Tan, Kevin McMillan, Yee Chan, Paul Manohar, Joe Thomas, Huong Ho, Peter Orio, Emily Holt, Margaret Cokelek, Nathan Lawrentschuk, Farshad Foroudi and Michael Chao
Soc. Int. Urol. J. 2024, 5(2), 111-121; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020020 - 16 Apr 2024
Abstract
►▼
Show Figures
Objectives: Our objective was to assess the rate of complications and gastrointestinal adverse effects of rectal spacer insertion for salvage post prostatectomy radiation therapy. Methods: A retrospective observational study was performed. Between September 2018 and March 2022, 64 post-radical prostatectomy patients who were
[...] Read more.
Objectives: Our objective was to assess the rate of complications and gastrointestinal adverse effects of rectal spacer insertion for salvage post prostatectomy radiation therapy. Methods: A retrospective observational study was performed. Between September 2018 and March 2022, 64 post-radical prostatectomy patients who were planned for salvage radiation therapy received a rectal spacer. The selected patients were those who had nerve-sparing prostatectomy with intrafascial or interfascial dissections (where Denonvillier’s fascia is retained). Radiation dose to the rectal wall and gastrointestinal symptoms were assessed. Symptoms were graded using the National Cancer Center Institute Common Terminology Criteria for Adverse Events v4.0 grading scheme. A total of 39 patients had pre-spacer planning computer tomography (CT) scans, and the rectal dose before and after the spacer insertion was calculated. Comparisons were made using the Student’s t-test, with a p-value < 0.05 representing statistical significance. Finally, clinicians were surveyed to rate the ease of the procedure using a 5-point Likert scale of 1 to 5 (1: very difficult, 2: difficult, 3: moderate, 4: easy, 5: very easy). Results: A total of 64 patients successfully underwent rectal spacer insertion. The mean age was 64.4 years (standard deviation: 5.7 years). After a median of 14 months’ (range 6 to 35) follow up, acute grade 1 and above gastrointestinal (GI) toxicities were seen in 28% of patients (grade 2 in 1.5%), and late grade 1 and above GI toxicities were seen in 12% of patients (grade 2 in 1.5%). Amongst the 39 patients with pre-spacer planning CT images, the volume of the rectum receiving 60%, 70%, 80%, 90%, and 100% of the prescribed radiation dose was reduced by 25.9%, 34.2%, 35.4%, 43.7%, and 61.7%, respectively. All dose reductions were statistically significant. The procedure was rated as “easy” or “very easy” to perform in 56% of cases. Conclusions: The insertion of a rectal spacer in selected patients undergoing PPRT is feasible and safe and significantly improves rectal wall radiation dosimetry in salvage post prostatectomy radiation therapy. It was accomplished in >95% of patients, increasing vesico-rectal separation from ‘immediate vicinity’ to 11 mm without any post-operative complications in experienced hands. In addition, it achieved significant reduction in rectal radiation doses, leading to low rates of acute and late grade 2 toxicity.
Full article
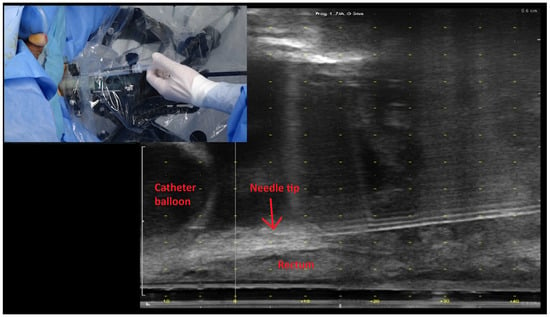
Figure 1
Open AccessGiants in Urology
Dr. Samuel Henry (Harry) Harris (22 August 1881 to 25 December 1936)
by
Darshan Sitharthan and Andrew Mitterdorfer
Soc. Int. Urol. J. 2024, 5(2), 108-110; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020019 - 12 Apr 2024
Abstract
In the original article [...]
Full article
Open AccessCommunication
Can Artificial Intelligence Treat My Urinary Tract Infections?—Evaluation of Health Information Provided by OpenAI™ ChatGPT on Urinary Tract Infections
by
Kevin Yinkit Zhuo, Paul Kim, James Kovacic, Venu Chalasani, Krishan Rasiah, Stuart Menogue and Amanda Chung
Soc. Int. Urol. J. 2024, 5(2), 104-107; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020018 - 11 Apr 2024
Abstract
Urinary tract infections (UTIs) are highly prevalent and have significant implications for patients. As internet-based health information becomes more relied upon, ChatGPT has emerged as a potential source of healthcare advice. In this study, ChatGPT-3.5 was subjected to 16 patient-like UTI queries, with
[...] Read more.
Urinary tract infections (UTIs) are highly prevalent and have significant implications for patients. As internet-based health information becomes more relied upon, ChatGPT has emerged as a potential source of healthcare advice. In this study, ChatGPT-3.5 was subjected to 16 patient-like UTI queries, with its responses evaluated by a panel of urologists. ChatGPT can address general UTI questions and exhibits some reasoning capacity in specific contexts. Nevertheless, it lacks source verification, occasionally overlooks vital information, and struggles with contextual clinical advice. ChatGPT holds promise as a supplementary tool in the urologist’s toolkit, demanding further refinement and validation for optimal integration.
Full article
Open AccessCommunication
Beware of Bipolar Transurethral Resection of Prostate in Patients with Previously Inserted Metallic Prostate Stapling Devices
by
Jianliang Liu, Nathan Lawrentschuk and Dixon T. S. Woon
Soc. Int. Urol. J. 2024, 5(2), 101-103; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020017 - 10 Apr 2024
Abstract
►▼
Show Figures
Metallic prostate stapling (e.g., UroLift) is a minimally invasive treatment option for men with bladder outlet obstruction from benign prostatic hyperplasia (BPH). While it provides rapid relief and preserves sexual function, unexpected interactions with other medical devices can compromise surgical procedures. In this
[...] Read more.
Metallic prostate stapling (e.g., UroLift) is a minimally invasive treatment option for men with bladder outlet obstruction from benign prostatic hyperplasia (BPH). While it provides rapid relief and preserves sexual function, unexpected interactions with other medical devices can compromise surgical procedures. In this letter, we highlight five cases where stapled metallic implants resulted in damage to bipolar energy device during transurethral resection of the prostate (TURP) and stimulation of obturator nerve. Laser may also reflect off metallic prostate implants which can result in laser equipment malfunction. Monopolar TURP should be considered in patients with existing metallic prostate implants who need further transurethral surgery for obstructive BPH to prevent bipolar instrument damage and obturator kick.
Full article
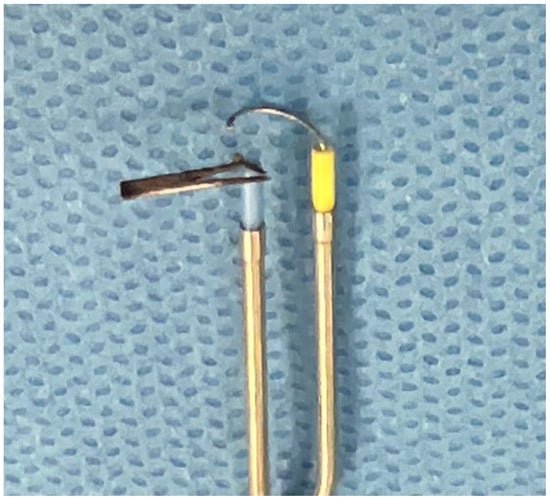
Figure 1
Open AccessCommentary
Smoking Cessation Tools in the Urological Context: Considering the Genitourinary Impacts of Smoking Cessation Tools
by
Nilanga Aki Bandara, Xuan Randy Zhou, Abdullah Alhamam, Peter C. Black and Marie-Pier St-Laurent
Soc. Int. Urol. J. 2024, 5(2), 97-100; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020016 - 09 Apr 2024
Abstract
Electronic cigarette use is rising globally. Although it may represent a potential smoking cessation tool, amidst misinformation and social media promotion, there is a growing concern regarding the health risks associated with its usage. These risks include adverse effects on the genitourinary system.
[...] Read more.
Electronic cigarette use is rising globally. Although it may represent a potential smoking cessation tool, amidst misinformation and social media promotion, there is a growing concern regarding the health risks associated with its usage. These risks include adverse effects on the genitourinary system. This commentary investigates the genitourinary effects of approved smoking cessation tools versus electronic cigarettes, urging urologists to prioritize established methods over electronic cigarettes due to their potential for multisystem toxicity and uncertain long-term health implications. Further research is warranted to evaluate comprehensively the genitourinary effects of these interventions.
Full article
Open AccessInteresting Images
The “Spiked Helmet Sign”, a Mimic of ST-Elevation Myocardial Infarction in Post-Nephrectomy Ileus
by
Jessica Wynn, Jonathan McCafferty and Robert Forsyth
Soc. Int. Urol. J. 2024, 5(2), 93-96; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020015 - 04 Apr 2024
Abstract
►▼
Show Figures
There are many causes of ST-elevation on electrocardiogram (ECG). ECG changes in the setting of intra-abdominal pathology is a rare and under characterised and includes the “spiked helmet sign”. We report a rare case of the “spiked helmet sign” that presented with ST-elevation
[...] Read more.
There are many causes of ST-elevation on electrocardiogram (ECG). ECG changes in the setting of intra-abdominal pathology is a rare and under characterised and includes the “spiked helmet sign”. We report a rare case of the “spiked helmet sign” that presented with ST-elevation in the precordial leads due to post-operative ileus.
Full article
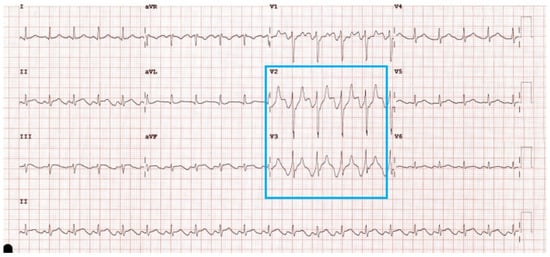
Figure 1
Open AccessArticle
Is the Bulbar Urethral Stricture a Single and Uniform Disease?
by
Tadashi Tabei, Akio Horiguchi, Masayuki Shinchi, Yusuke Hirano, Kenichiro Ojima, Keiichi Ito and Ryuichi Azuma
Soc. Int. Urol. J. 2024, 5(2), 85-92; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5020014 - 04 Apr 2024
Abstract
►▼
Show Figures
Objectives: Proximal and distal bulbar urethral strictures (BUS) have different disease characteristics and require different treatment strategies despite being regarded as a single condition. To clarify the differences, we analyzed our database by distinguishing the two types of BUS. Methods: We retrospectively reviewed
[...] Read more.
Objectives: Proximal and distal bulbar urethral strictures (BUS) have different disease characteristics and require different treatment strategies despite being regarded as a single condition. To clarify the differences, we analyzed our database by distinguishing the two types of BUS. Methods: We retrospectively reviewed the data of 196 patients with BUS who underwent urethroplasty at the National Defense Medical College (Japan) between August 2004 and March 2022. We divided patients into proximal (group 1) or distal (group 2) groups based on the stricture segment and compared patient background and surgical techniques for each group. We assessed whether the stricture segment was an independent predictive factor for substitution urethroplasty selection using multivariate logistic regression analysis. The recurrence rates were calculated and compared using the Kaplan–Meier method and log-rank test, respectively. Results: Patients in group 1 had a less frequent non-obliterated lumen (73% vs. 94%, p = 0.020) and significantly shorter strictures (10 mm vs. 23 mm, p < 0.001) more frequently caused by external traumas (47% vs. 26%, p = 0.010) than those in group 2. Logistic regression analysis revealed that the stricture segment (distal) (p < 0.001), stricture length (≥20 mm) (p < 0.001), ≥2 prior transurethral procedures (p = 0.030), and a non-obliterated lumen (p = 0.020) were independent predictive factors for substitution urethroplasty. However, the recurrence rate (p = 0.18) did not significantly differ between the two groups. Conclusions: Proximal and distal BUS have substantially different anatomical characteristics and etiologies and require different reconstructive techniques.
Full article
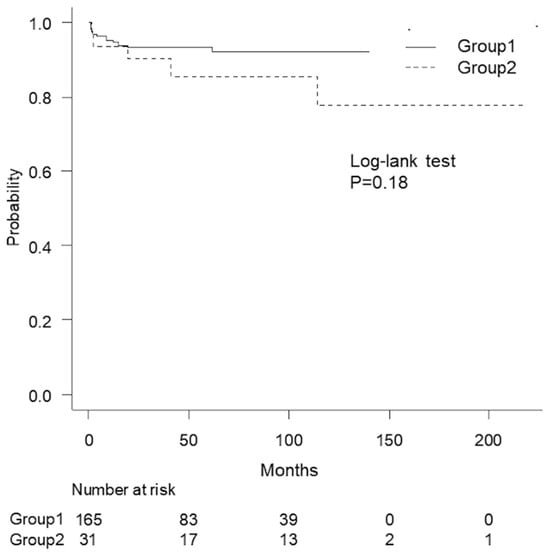
Figure 1
Open AccessArticle
Robotic Precision vs. Human Dexterity—Benchtop Comparative Study of Free-Hand vs. Robotic-Assisted Puncture in Fluoroscopy-Guided Percutaneous Nephrolithotomy
by
Jeffery Ze Kang Lim, Chai Chu Ann, Aung Kyaw Phyo, Kanesh Kumaran, Ahmad Nazran, Shanggar Kuppusamy, Teng Aik Ong and Wei Sien Yeoh
Soc. Int. Urol. J. 2024, 5(1), 76-84; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5010013 - 19 Feb 2024
Abstract
►▼
Show Figures
Introduction: Percutaneous nephrolithotomy (PCNL) is the standard procedure for treating large kidney stones, especially those measuring over 20 mm or staghorn stones. Accurate placement of the tract into the renal collecting system of interest is crucial. Objective: To compare the free-hand puncture technique
[...] Read more.
Introduction: Percutaneous nephrolithotomy (PCNL) is the standard procedure for treating large kidney stones, especially those measuring over 20 mm or staghorn stones. Accurate placement of the tract into the renal collecting system of interest is crucial. Objective: To compare the free-hand puncture technique with robotic-assisted puncture during fluoroscopy-guided PCNL on a phantom kidney model in terms of efficiency and safety. A self-assessment of confidence levels after each puncture was recorded. Study Design: This prospective single-center benchtop study was conducted at the University Malaya Medical Centre (UMMC). Four urological residents participated and performed phantom punctures using both the free-hand bull’s eye technique and the automated needle targeting system with X-ray (ANT-X). Each resident performed a total of 60 punctures on the renal phantom models, with 30 punctures using the free-hand technique and 30 punctures using the ANT-X robotic-assisted system. Results: A total of 240 needle insertions were conducted, with 120 in the ANT-X group and 120 in the free-hand group. The success rate of needle insertions was 100% in both groups. However, the study revealed that the ANT-X group required, on average, an additional 51 s for needle puncture compared to the free-hand group (p < 0.001). In terms of fluoroscopic exposure, the ANT-X group exhibited significantly lower radiation exposure compared to the free-hand group (p < 0.001). Sub-analysis showed that puncture time remained consistent regardless of the technique used, but fluoroscopic screening time decreased with increasing participant experience. The ANT-X group also resulted in significantly lower radiation exposure during initial sessions compared to the free-hand technique. Surgeons’ self-assessment of confidence levels indicated a high level of confidence in needle puncture. Conclusions: Our benchtop study comparing the efficacy and safety between free-hand and ANT-X phantom punctures revealed comparable results. The needle puncture technique facilitated by the ANT-X system showed promising results in terms of reducing fluoroscopic exposure, albeit at the cost of longer operative times. This technology holds promise for novice surgeons who are in the early stages of their learning curve and might be useful for experienced surgeons looking to reduce radiation exposure.
Full article
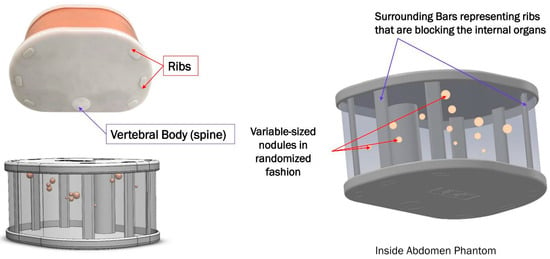
Figure 1
Open AccessSystematic Review
Ultrasound-Based Prognostic Anatomical Parameters for Post-Prostatectomy Incontinence: A Systematic Review
by
Cecile T. Pham, Jordan E. Cohen and Manish I. Patel
Soc. Int. Urol. J. 2024, 5(1), 64-75; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5010012 - 18 Feb 2024
Abstract
►▼
Show Figures
Background: A number of assessment methods for the pelvic floor have been described. Male pelvic floor ultrasound is an accessible, noninvasive assessment tool. Objective: To evaluate current published literature on anatomical parameters on pre- and postoperative ultrasound imaging of the male pelvic floor
[...] Read more.
Background: A number of assessment methods for the pelvic floor have been described. Male pelvic floor ultrasound is an accessible, noninvasive assessment tool. Objective: To evaluate current published literature on anatomical parameters on pre- and postoperative ultrasound imaging of the male pelvic floor and correlation with continence status following radical prostatectomy (RP). Methods: A comprehensive literature search was conducted using the PRISMA guidelines to identify publications up to November 2022. Exclusion criteria consisted of animal studies, non-English articles, case reports, reviews and abstracts or reports from conferences. A full-text review was performed on 12 papers using ultrasound to assess pelvic floor anatomy and correlation with continence status following RP. Results: A total of 18 anatomical parameters were evaluated using US. Membranous urethral length (MUL), striated urethral sphincter (SUS) morphology and activation were most commonly studied. Shorter pre- and postoperative MUL, decreased preoperative SUS thickness and vascularity, postoperative discontinuity of SUS muscle fibres and decreased SUS activation are associated with post-prostatectomy incontinence (PPI). There is a paucity of data comparing anatomical changes in men prior to and following RP. The benefits of transperineal ultrasound are that it is minimally invasive, accessible, provides dynamic imaging of all three striated muscle complexes simultaneously and includes a bony landmark to reference measures of pelvic floor muscle displacement. Conclusions: Ultrasound evaluation of the male pelvic floor is an evolving field as there is development in technology and understanding of pelvic floor anatomy. It is an accessible and dynamic imaging modality, which allows both morphological and functional assessment of pelvic floor anatomy and its role in PPI. MUL and SUS morphology and activation are associated with continence status following RP. Several other anatomical parameters that may predict PPI were identified. Current literature is limited by small, single-centre studies with heterogeneous cohorts and methodologies.
Full article
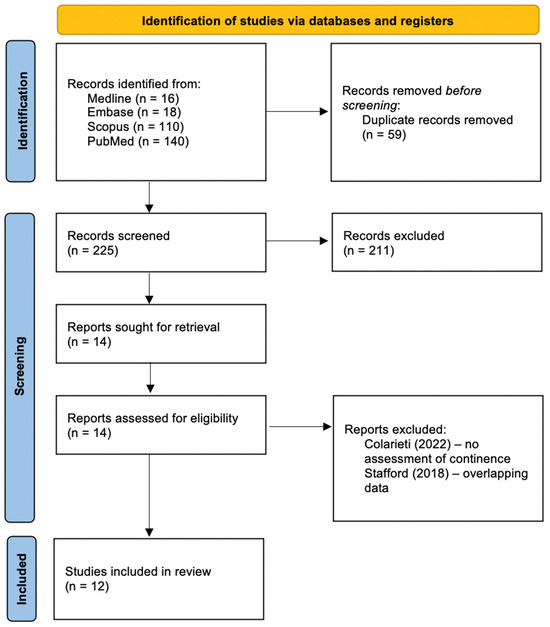
Figure 1
Open AccessArticle
Safety and Efficacy of Bilateral Tubeless Supine Mini-Percutaneous Nephrolithotomy for the Management of Bilateral Renal Calculi in Renal Failure Patients
by
Puvai Murugan Ponnuswamy, Bhalaguru Iyyan Arumugam, Shree Vishnu Siddarth Rajagopal and Krishna Mohan Boopathy Vijayaraghavan
Soc. Int. Urol. J. 2024, 5(1), 56-63; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5010011 - 18 Feb 2024
Abstract
►▼
Show Figures
Background: To evaluate the safety, efficacy, feasibility, stone-free rate, and complications of bilateral tubeless supine mini-percutaneous nephrolithotomy (M-PCNL) for bilateral multiple renal calculi with renal failure as a single-stage procedure. Materials and Methods: We conducted a retrospective study from January 2020 to March
[...] Read more.
Background: To evaluate the safety, efficacy, feasibility, stone-free rate, and complications of bilateral tubeless supine mini-percutaneous nephrolithotomy (M-PCNL) for bilateral multiple renal calculi with renal failure as a single-stage procedure. Materials and Methods: We conducted a retrospective study from January 2020 to March 2022 in adult patients with bilateral renal or proximal ureteric calculi with renal failure who were subjected to bilateral supine tubeless M-PCNL. Patients on regular hemodialysis before the procedure were excluded. Data regarding the demographic profile, stone characteristics on non-contrast computed tomography (NCCT), duration of surgery, complications, and auxiliary procedures were retrieved from clinical records. Residual stone fragments of≤4mm in NCCT were considered clinically insignificant. The Clinical Research Office of the Endourological Society validation ofClavien score for PCNL complications was used. Results: A total of twenty-seven patients with a mean age of 45.9years were included in this study. The mean size of stone diameter per renal unit was 2.4 ± 0.4 cm. The mean preoperative serum creatinine was 2.8 mg/dL. A total of 62 tracts and 27 sessions were required for complete treatment of all 54 renal units in the 27 successfully treated patients. The average operating time was 75 (52–122) min on both sides. Serum creatinine drop at onemonth postsurgery was statistically significant (p < 0.0001). Mean hospitalization time was 3.6 days [3–6 days]. The primary stone-free rate was 92.5%. Grade I, II, and IVA complications were recorded in three (11.1%), eight (29.6%), and two (7.4%) patients, respectively. Conclusion: Bilateral tubeless supine M-PCNL for bilateral renal calculi in selective patients with renal failure in a single session is a safe, feasible, and effective option which can be carried out without increased morbidity and can be attempted if the first-side M-PCNL has gone smoothly within a reasonable amount of time.
Full article
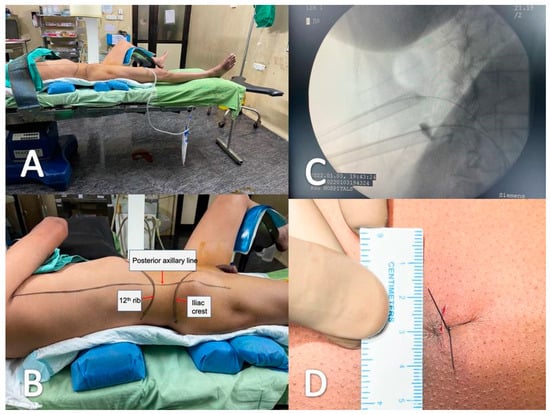
Figure 1
Open AccessCommentary
Accessibility to Andrology Medical Devices in Arab-Muslim Countries
by
Mounir Jamali
Soc. Int. Urol. J. 2024, 5(1), 54-55; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5010010 - 17 Feb 2024
Abstract
Highlighting the restricted access to andrology medical devices in Arab Muslim countries, where unjust associations with sexual instruments lead to prohibitions, this commentary underscores the challenges in providing appropriate medical care for andrological conditions. Despite the crucial role of devices like penile extenders,
[...] Read more.
Highlighting the restricted access to andrology medical devices in Arab Muslim countries, where unjust associations with sexual instruments lead to prohibitions, this commentary underscores the challenges in providing appropriate medical care for andrological conditions. Despite the crucial role of devices like penile extenders, vacuum devices, and vibrators in treating conditions such as Peyronie’s disease and erectile dysfunction, cultural and religious biases condemn them in certain regions. This lack of understanding deprives many patients of andrological treatments, limiting therapeutic options and equitable healthcare access. The commentary advocates for urology societies to raise awareness, engage policymakers, and use media to distinguish these devices from sex toys, emphasizing their medical nature for the benefit of patients.
Full article
Open AccessUrology around the World
Australian Kidney Transplantation in the Shadow of COVID-19: A Decade’s Insight
by
Darshan Sitharthan, Marco Rosario and Keeththana Thayanantharajah
Soc. Int. Urol. J. 2024, 5(1), 51-53; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5010009 - 16 Feb 2024
Abstract
►▼
Show Figures
The journey of organ transplantation in Australia has been marked with progressive milestones since the inaugural kidney transplant in 1965 [...]
Full article
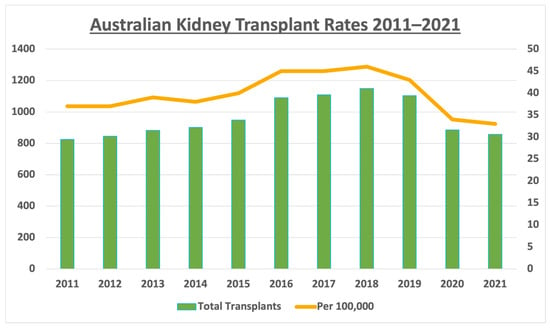
Figure 1
Open AccessArticle
Transfusion in Radical Cystectomy Increases Overall Morbidity and Mortality: A Retrospective Study Using Data from the American College of Surgeons—National Surgical Quality Improvement Program
by
Christian H. Ayoub, Nassib F. Abou Heidar, Alexandre K. Armache, Elia Abou Chawareb and Albert El Hajj
Soc. Int. Urol. J. 2024, 5(1), 42-50; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5010008 - 14 Feb 2024
Abstract
Background: Radical cystectomy is a complex procedure imposing significant post-operation complications. Objective: Explore the impact of peri-operative pRBC transfusion on mortality and overall morbidity in a matched cohort. Methods: The American College of Surgeons—National Surgical Quality Improvement Program’s (ACS-NSQIP) dataset was used to
[...] Read more.
Background: Radical cystectomy is a complex procedure imposing significant post-operation complications. Objective: Explore the impact of peri-operative pRBC transfusion on mortality and overall morbidity in a matched cohort. Methods: The American College of Surgeons—National Surgical Quality Improvement Program’s (ACS-NSQIP) dataset was used to select patients who underwent RC in 2008–2019. Patients who witnessed pre-operative transfusion and emergency cases were excluded. Peri-operative pRBC transfusion was defined as an intra-operative or up to 24-h post-operative pRBC transfusion. We matched patients who underwent peri-operative pRBC transfusion to patients who did not receive transfusion. Length of stay, mortality, and overall morbidity were compared between the two matched cohorts. Results: The match cohort was matched on all pre-operative demographics and medical history variables and yielded 3578 matched patients. Patients who underwent peri-operative pRBC transfusion had a longer length of hospital stay (9.3 days) as compared to patients who did not undergo transfusion (8.13 days) (p < 0.001). Furthermore, patients who underwent transfusion also had higher odds of mortality (OR = 1.934) and overall morbidity (OR = 1.443) (p < 0.03). Specifically, patients who underwent transfusion had higher odds of organ space SSI, pneumonia, unplanned intubation, pulmonary embolism, failure to wean off of ventilator, renal insufficiency, urinary tract infections, stroke, myocardial infarction, cardiac arrest requiring CPR, deep vein thrombosis, and septic shock (p < 0.047). Conclusion: Peri-operative pRBC transfusion in RC was associated with longer hospital stays, significant morbidity, and mortality. For this reason, pre-operative patient optimization and possible alternatives to common pRBC practices should be considered in RC to circumvent complications.
Full article
Open AccessArticle
Does Autologous Blood Injection Following Dextranomer/Hyaluronic Acid Copolymer Implantation in Treating Vesicoureteral Reflux Affect the Microsphere Particle Leakage?
by
Hooman Kamran, Nooshin Tafazoli, Sahar Eftekharzadeh, Pooya Hekmati, Hamid Arshadi and Abdol-Mohammad Kajbafzadeh
Soc. Int. Urol. J. 2024, 5(1), 31-41; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5010007 - 13 Feb 2024
Abstract
►▼
Show Figures
Objectives: It has been shown that concomitant autologous blood and dextranomer/hyaluronic acid (Deflux®) injection, hydrodistension autologous blood injection technique (HABIT), had a better mound preservation and treatment success compared to the hydrodistension injection technique (HIT) in vesicoureteral reflux (VUR) correction. In
[...] Read more.
Objectives: It has been shown that concomitant autologous blood and dextranomer/hyaluronic acid (Deflux®) injection, hydrodistension autologous blood injection technique (HABIT), had a better mound preservation and treatment success compared to the hydrodistension injection technique (HIT) in vesicoureteral reflux (VUR) correction. In this study, we aimed to show microscopically whether the concomitant injection of autologous blood decreases the leakage of Deflux® particles. Methods: Children with VUR who underwent HIT or HABIT between March 2020 and January 2023 were enrolled. Following the completion of the procedure on each ureter, the bladder was irrigated for 3 to 5 min, and the retrieved sample of irrigation fluid was evaluated for dextranomer particle count as “immediate leakage”. A Foley catheter was placed, and a urine sample after 12 h was collected as “early leakage”. Results: A total of 86 children with a median age of 3.0 years (interquartile range = 4.6) were included. Overall, 66 patients underwent HABIT, and 20 children underwent HIT. Rupture was observed in five patients during the procedure, and re-injection was conducted successfully in these cases. Immediate, early, and total particle leakage in the first 12 h of the injection were significantly less in the HABIT group compared to the HIT group. In the regression analysis, only the injection technique (HIT/HABIT) and rupture were significantly associated with the total particle leakage in the first 12 h. Conclusions: Immediate injection of autologous blood into the mound following an endoscopic correction of VUR in children is associated with significantly less Deflux® particle leakage from the injection site regardless of the VUR grade. We hypothesize that a concomitant blood injection into the Deflux® mound will create a blood clot while the needle is kept in situ and help to stabilize the mound and decrease treatment failure by minimizing particle leakage from the injection site.
Full article
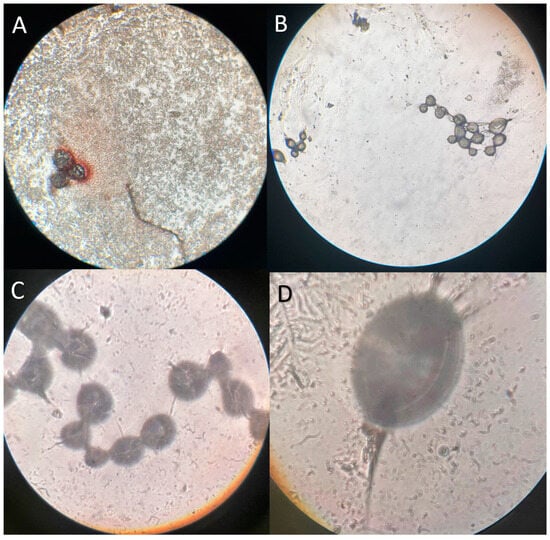
Figure 1
Open AccessReview
“Pass the Genetic Scalpel”: A Comprehensive Review of Clustered Regularly Interspaced Short Palindromic Repeats (CRISPR) in Urological Cancers
by
Arthur Yim, Matthew Alberto, Marco Herold, Dixon Woon, Joseph Ischia and Damien Bolton
Soc. Int. Urol. J. 2024, 5(1), 16-30; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5010006 - 13 Feb 2024
Abstract
►▼
Show Figures
Introduction: Urological cancers account for a significant portion of cancer diagnoses and mortality rates worldwide. The traditional treatment options of surgery and chemoradiation can have significant morbidity and become ineffective in refractory disease. The discovery of the CRISPR system has opened up
[...] Read more.
Introduction: Urological cancers account for a significant portion of cancer diagnoses and mortality rates worldwide. The traditional treatment options of surgery and chemoradiation can have significant morbidity and become ineffective in refractory disease. The discovery of the CRISPR system has opened up new avenues for cancer research by targeting specific genes or mutations that play a role in cancer development and progression. In this review, we summarise the current state of research on CRISPR in urology and discuss its potential for improving the diagnosis and treatment of urological cancers. Methods: A comprehensive literature search was conducted on databases including PubMed, Embase, and Cochrane Library. The keywords included CRISPR and urology OR prostate OR renal OR bladder OR testicular cancer. Results: CRISPR has been used extensively in a preclinical setting to identify and target genes in prostate cancer, including AR, NANOG, ERβ, TP53, PTEN, and PD-1. Targeting PRRX2 and PTEN has also been shown to overcome enzalutamide and docetaxel resistance in vitro. In bladder cancer, CBP, p300, hTERT, lncRNA SNGH3, SMAD7e, and FOXA1 have been targeted, with HNRNPU knockout demonstrating tumour inhibition, increased apoptosis and enhanced cisplatin sensitivity both in vitro and in vivo. Renal cancer has seen CRISPR target VHL, TWIST1, PTEN, and CD70, with the first in-human clinical trial of Anti-CD70 CAR T cell therapy showing an excellent safety profile and durable oncological results. Lastly, testicular cancer modelling has utilised CRISPR to knockout FLNA, ASH2L, HMGB4, CD24, and VIRMA, with NAE1 found to be over-expressed in cisplatin-resistant germ cell colonies. Conclusions: CRISPR is a cutting-edge technology that has been used extensively in the pre-clinical setting to identify new genetic targets, enhance drug sensitivity, and inhibit cancer progression in animal models. Although CAR T cell therapy has shown promising results in RCC, CRISPR-based therapeutics are far from mainstream, with further studies needed across all urological malignancies.
Full article
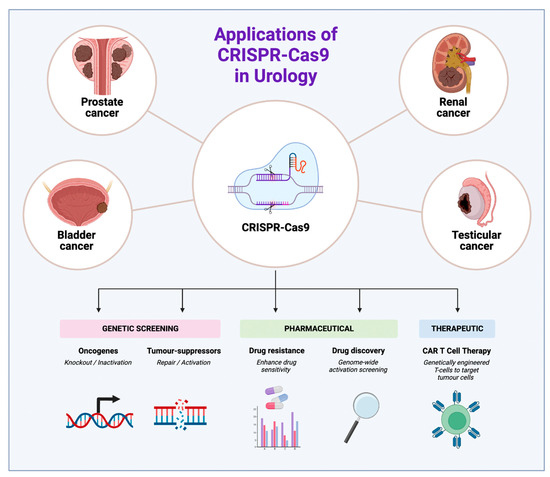
Figure 1
Open AccessArticle
A 10-Year Multicentre Experience of Australian Penile Fracture Repair Outcomes
by
Matthew Yii, Chrisdan Gan, Kirby R. Qin, Damien Bolton and Gideon Blecher
Soc. Int. Urol. J. 2024, 5(1), 10-15; https://0-doi-org.brum.beds.ac.uk/10.3390/siuj5010005 - 13 Feb 2024
Abstract
Objectives and Methods: Penile fractures are a urologic emergency involving the rupture of the tunica albuginea of the corpora cavernosum. Geography is known to impact fracture aetiology, and higher impact aetiology is thought to predispose patients to complex trauma. To review long-term urinary
[...] Read more.
Objectives and Methods: Penile fractures are a urologic emergency involving the rupture of the tunica albuginea of the corpora cavernosum. Geography is known to impact fracture aetiology, and higher impact aetiology is thought to predispose patients to complex trauma. To review long-term urinary and sexual outcomes following fracture repair in Australia, a retrospective analysis of data from three metropolitan hospital services over 10 years was performed. Only patients with intraoperatively confirmed fractures were included. Patients were contacted by clinicians to complete a survey, which utilised validated questionnaires, including the International Index of Erectile Function-5 (IIEF-5) and the International Prostate Symptom Score (IPSS). Perioperative data were analysed against survey responses. Results: We identified 55 confirmed penile fractures. Twenty-one patients completed questionnaire follow-ups, comprising the study cohort. The median age at the time of the injury was 44.8 years (range: 25–65). The median time from injury to questionnaire completion was 4.0 years (range: 1–10). Furthermore, 95.5% (20) of the injuries occurred during sexual intercourse. The median IIEF-5 score was 23 (range: 5–25); the median IPSS score was 5 (range: 0–22). Seven patients (33.3%) sustained a bilateral cavernosal injury, and eight (38.1%) sustained a urethral injury. Upon conducting a Mann–Whitney U test, no significant relationships were found between bilateral cavernosal injury and IIEF-5 scores (p = 0.7377) or urethral injury and IPSS scores (p = 0.5338). Conclusions: The Australian aetiology of penile fractures appears consistent with that of other Western countries, with subsequent high rates of bilateral cavernosal and urethral injuries. The long-term erectile and urinary function outcomes observed are promising. A larger prospective study would further illuminate the relationship between injury factors and outcomes, revealing information not presented herein due to study limitations relating to the cohort size and follow-up rates.
Full article
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics